In 1943, the Austrian psychiatrist Leo Kanner studied children with unusual behavior patterns that avoided eye contact and had bad or not developed the ability to speak. He first described the disorder that we know today as autism. Back then, autism was considered as a form of mental retardation and/or insanity. American psychiatrist and writer Harlan Lane in his book “The Wild Boy of Aveyron” (Harvard University Press, 1979) described the case of an autistic boy Victor, who lived in the 19th century and was found solitary wandering the woods near Toulouse in France. Although apparently physically healthy boy with badly developed communication skills and anti-social behavior, doctors and scientists who have begun to study his behavior could not say that he was mentally retarded nor insane.
The term autism was created in the 19th century when it was first used by Swiss physician Eugen Bleuler. He wanted to describe patients who have suffered from exaggerated desire to escape from reality. Leo Kanner took over this term because he believed that the children, whose behavior he studied, also wanted to get away from the reality that surrounded them and to shut themselves into some of their imaginary world.
 Today, autism is defined as a developmental disorder of still unknown etiology, that occurs at birth or within the first three years of age, which does not always at first become fully apparent. Most autistic children are physically completely healthy and normal, but there is an unusual pattern of behavior that differs them from other children, and usually involves the absence of normal and understandable speech and avoiding eye contact. A milder form of autism in which children have the capability of normal speech is called Asperger’s syndrome.
Today, autism is defined as a developmental disorder of still unknown etiology, that occurs at birth or within the first three years of age, which does not always at first become fully apparent. Most autistic children are physically completely healthy and normal, but there is an unusual pattern of behavior that differs them from other children, and usually involves the absence of normal and understandable speech and avoiding eye contact. A milder form of autism in which children have the capability of normal speech is called Asperger’s syndrome.
Some specific behavioral characteristics and peculiarities of conduct by which one can recognize a child with autism include:
- difficulties with social relationships,
- difficulties in communication,
- difficulties in playing and imagining,
- resisting to changes in the daily routine,
- rejection of physical contact,
- the lack of attention and concern for others,
- the lack of eye contact,
- refusal of playing and communicating with other children,
- strikingly hyperactive or extremely passive behavior,
- the lack of fear of danger situations,
- laughing or giggling for no reason,
- repetitive moving of objects or parts of the body,
- resistance to learning,
- the mechanical repetition of words,
- unimaginative in playing,
- an unusual attachment and preoccupation with specific objects.
Diagnosis of autism is made based on the results of the medical, psychological and neurological tests. To diagnose an autism, four criteria should be met:
- pronounced abnormality in reciprocal social relations,
- pronounced abnormality in the development of communication skills including speech,
- restricted, repetitive and stereotyped patterns of behavior, activities and imagination,
- early appearance of the first signs of disorder (between the first and third year of life).
It is believed that on 10,000 newborns, 4 to 5 children are born with autism. When it comes to spectrum of autistic disorders, it is about 10 to 15 children per 10,000 newborns. Autism often affects boys than girls.
 Considering that going to the dentist is something that is not part of the child’s daily routine, it can cause many troubles in children with autism and their parents or guardians. The fear that appears in autistic individuals can lead to severe panic attacks that prevent the performance of dental procedures. In addition, autistic children are extremely sensitive to bright light, new sounds, smells, tastes and colors, which are often stimuli that necessarily arise during dental visits and performing dental procedures. As the number of patients with autism is relatively small compared to the number of patients with other diseases, the preservation of their oral health is the task the dentist does not encounter often with. Due to the specifics of the autistic disorder, this is a special challenge that requires not only knowledge and skills, but also a lot of patience.
Considering that going to the dentist is something that is not part of the child’s daily routine, it can cause many troubles in children with autism and their parents or guardians. The fear that appears in autistic individuals can lead to severe panic attacks that prevent the performance of dental procedures. In addition, autistic children are extremely sensitive to bright light, new sounds, smells, tastes and colors, which are often stimuli that necessarily arise during dental visits and performing dental procedures. As the number of patients with autism is relatively small compared to the number of patients with other diseases, the preservation of their oral health is the task the dentist does not encounter often with. Due to the specifics of the autistic disorder, this is a special challenge that requires not only knowledge and skills, but also a lot of patience.
Although autistic persons mostly are not mentally disabled persons and can even have a very high IQ, usually they are not prone to learning and acquiring new knowledge and skills, or it takes a lot more time than for healthy people. This is a problem in the development of many abilities, including the developing of habits of oral hygiene. Therefore, the application of preventive measures and regular dental visits are especially important for these persons.
Oral health in children with autism
Autism does not cause specific changes in the mouth and usually has no direct impact on oral health. But certain peculiarities in the behavior of autistic persons can significantly affect their oral health. This primarily refers to a reduced ability to learn and correctly apply oral hygiene measures and preference for repetitive behavior that, in certain forms of behavior, can lead to self-injuring of structures of the oral cavity. A failure to adopt the habits of regular and proper maintenance of oral hygiene leads to accumulation of plaque, tartar and occurrence of tooth decay, which can lead to inflammation of the dental pulp and more complex forms of dental diseases.
The incidence of dental caries in autistic individuals has been the subject of numerous studies which were meant to determine whether there is a difference in the incidence of caries between autistic and healthy individuals. Although we can not unanimously say that the prevalence of dental caries in autistic individuals is increased, a high correlation between appropriate care for the autistic person and oral health was revealed. This means that patients whose parents or guardians are familiar with the nature of the disorder and thus found an appropriate way for quality and regular implementation of oral hygiene measures have a lower number of caries teeth and better oral health.
In addition to caries is caries-related pathological changes, in autistic individuals oral self-injuries may occur. Most cases of oral self-injuries happen in children and adolescents, while they are rare in the adult population. Oral self-harm includes: tooth avulsion (tooth completely knocked out) of mostly milk teeth (a situation where a child looses and pulls tooth), oral ulcers, biting the cheeks, tongue or lips, creating injuries on the oral cavity structures such as gums and mucous membranes. Oral self-injury is an extremely complex problem whose treatment requires a multidisciplinary approach that, beside a parent or guardian, also includes dentists, psychologists and psychiatrists. Namely, by causing such injuries, which can sometimes seem very dramatic, autistic person attracts attention and thus expresses a wish or need. There were recorded cases where a child was pounding his head against the wall for days, until parents realized that he had a toothache. There are no universal solutions to deal with such situations. The dentist must treat each patient separately and try to better understand the relationships within the patient’s family after the compulsory establishment of trust between himself and the patient.
 Oral preventive measures for autistic children
Oral preventive measures for autistic children
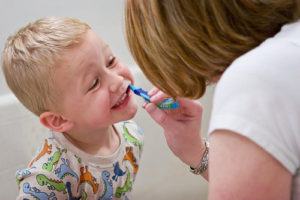
Oral preventive measures for autistic people and children do not differ from the preventive measures that are usually recommend for other, healthy people. These measures include properly and regularly conduct of oral hygiene, teeth fluoridation, preventive fissure sealing of teeth in children, tips on proper nutrition and of course regular visits to the dentist. Considering that autistic people usually show a low ability to embrace changes, their education on oral hygiene measures is usually long and difficult.
The changes should be introduced gradually and step by step in order to cross into the habit and become a kind of everyday ritual. For example, learning how to brush teeth should be done on a daily basis, and should be taught in such a way that the first a toothbrush should be given to a child to play with it in a place where normally resides. When a child accepts to play with toothbrush, it should be taken into the bathroom and allowed to be in this “new” space to play with electric toothbrush for kids. After accepting this, while the child is in the bathroom, the next step is to soak the toothbrush with water and give it to the child to put in it’s mouth, and then gently rub the teeth. When this second step is overcome, a toothpaste should be put on toothbrush and again suggest to the child that it should rub it’s teeth.

Although this process may be extended to even a few weeks, and sometimes more, it eventually leads to that the child independently brushes it’s teeth, because brushing is now a new routine. Every step and every good behavior of the child must be accompanied by praise, approval and possibly symbolic rewards. Sometimes some aids made according to the principles of visual pedagogy can help. The most common are paintings and illustrations which, in an understandable way for a child, show the actions and the behavior that should be adopted. The images that illustrate the process of brushing have proven to be extremely useful with a large number of autistic children.
Autistic children often have an emphasized need for sweets and pureed food, whose consummation contributes to the development of caries, especially in circumstances of insufficient maintenance of oral hygiene. So the dentist should advise parents about proper nutrition, which should include as many raw fruits and vegetables and less refined carbohydrates, carbonated and sweetened drinks. Only exceptionally, sweets may serve as a reward for good behavior.
A visit to the dentist
Visit to the dentist can be extremely traumatic for the patients with autism and their escort, and above all exhausting for dentists and dental staff. This is one of the reasons why the most common dental procedure in this group of patients is tooth extraction. Unfortunately, these patients usually come to the dentist only when the pain becomes unbearable and the tooth extraction is the only possible solution. Although dental procedures and treatments in autistic individuals do not differ from those in healthy individuals, it is recommended to visit a dentist who is a specialist in pediatric dentistry. He is especially trained to deal with such patients and know in advance what are the possible complications and adapts to perform the necessary dental procedures.
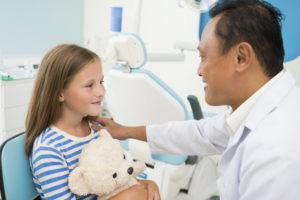
In order that the visit to the dentist would not be a traumatic experience and counterproductive, parents and dentist should ensure this becomes a kind of habit for autistic person. Studies have shown that such children should be taken to the dentist once every week and slowly get used to the new environment and people. Of course, the performance of dental procedures should also be gradual. The child should first learn to open it’s mouth and keep it open as long as possible. After a while, when a relationship between the child and the dentist is established, the child will when arrives in dental office open it’s mouth and allow the dentist to perform the necessary procedure. The dentist will need to align his actions with a degree of confidence that the child has developed and should first perform simple and painless procedures such as tooth brushing and coating teeth with formulations of fluoride. After these procedures, the dentist should gradually transfer to the rehabilitation of carious lesions.
It is advised that performing the procedure takes no more than 30 minutes. Given the fact that autistic children respond well to the method of “tell-show-do”, any action the dentist should first describe in words, show to the child, and then carry out. If the child behaves well and cooperatively, it should be rewarded. If the child’s behavior is unsatisfactory then the reward should not be given.
If the child is extremely uncooperative, and a technique of forming the child’s behavior did not give the desired results, in order to deprive a child from pain and discomfort that tooth decay causes, the dentist should consider the possibility of performing dental procedures in sedation or under general anesthesia or in sedation. General anesthesia is a solution that is applied when all other possibilities have been exhausted, and dental treatment is necessary and inevitable.
Conclusion
Autism is a complex disorder that often inhibits the ability to communicate, respond to surrounding stimuli and create relationships with other people. Due to the difficulty in acceptance of changes in the daily routine and less willingness to learn, oral health in children with autism is usually affected by faulty implementation of oral hygiene measures. This may encourage the formation of cavities, tartar buildups and changes in the gums and oral mucosa. In order to avoid the occurrence of these oral diseases it is recommended, despite the initial resistance, to teach the child to brush it’s teeth and that the child gets used to regularly visit the dentist. Although the road to healthy teeth and mouth of an autistic child is long and difficult, but it is not impossible and unattainable. It requires patience and persistence from both parents and dentist.