Table of Contents
Orofacial pain can be defined as any pain that occurs in the face and mouth, including the nose, ear, eye and throat. It affects millions of people every day around the world, and can be caused by a variety of disorders and diseases. Orofacial pain can be divided into odontogenic and nonodontogenic pain.
Odontogena pain is any pain in the face and mouth caused by tooth (Gr. Odous = tooth), while neodontogena pain any pain in that area which is not of dental origin (lat. dens = tooth). Although the definition of dental pain is clear and simple, its interpretation and classification vary from author to author. Some authors odontogenic pain shared by only the dentin and pulp pain, while some that divide add more and periodontal pain, periapical pain and reflected pain, depending on which part of the tooth or the corresponding tissue causes.
What are the causes of dental pain?
Factors that adversely affect the integrity, physiology and normal functioning teeth can cause odontogenic pain. These factors may act on a tooth and the pulp or supporting system tooth and periapical tissue. Factors that affect the tooth and the pulp and causing odontogenic pain can be bacterial, traumatic, iatrogenic, chemical and idiopathic nature. They can cause inflammation of the pulp (temporary and permanent) or its necrosis and withering away.
The microorganisms that are found in dental caries are the most common bacterial causes of changes in the dental pulp, and thus dental pain. Acute (crown and root fractures, loosening and tooth avulsion) and chronic (teeth grinding, attrition, abrasion, erosion) dental trauma caused by the current odontogenic pain, or painful sensation that is slowly evolving and becoming more pronounced. Many dental procedures of cleaning cavities, restoring, through grinding teeth for prosthetic, to orthodontic movement of teeth can cause iatrogenic odontogenic pain. Additionally, dental materials applied on or near the pulp can cause painful stimuli.
Sometimes odontogenic pain can not find the real cause, we are talking about idiopathic odontogenic pain. However, there are conditions and diseases for which there is reasonable suspicion that may manifest as a painful sensation in the teeth. In this respect, the most frequently mentioned aging, internal and external resorption of teeth, hereditary hypophosphatemia, sickle cell anemia, herpes zoster infections and AIDS.
How to identify odontogenic pain?
- Grab this awesome groovy tie dye design present shirt for dentists, dental Assistants, dental school students, and Assistants. Great birthday idea for promoting the benefits of fighting tooth decay with floss and flouride.
- Dentist Groovy Dental Orofacial pain Design For Dental Dentist apparel birthday
- This premium t-shirt is made of lightweight fine jersey fabric
- Fit: Men’s fit runs small, size up for a looser fit. Women’s fit is true to size, order usual size.
- Grab this awesome groovy tie dye design present shirt for dentists, dental Assistants, dental school students, and Assistants. Great birthday idea for promoting the benefits of fighting tooth decay with floss and flouride.
- Dentist Groovy Dental Orofacial pain Design For Dental Dentist apparel birthday
- Lightweight, Classic fit, Double-needle sleeve and bottom hem
- Grab this awesome groovy tie dye design present shirt for dentists, dental Assistants, dental school students, and Assistants. Great birthday idea for promoting the benefits of fighting tooth decay with floss and flouride.
- Dentist Groovy Dental Orofacial pain Design For Dental Dentist apparel birthday
- Lightweight, Classic fit, Double-needle sleeve and bottom hem
Odontogena pain sometimes can be readily and easily identify, and sometimes the procedure was extremely difficult and complex. Odontogena pain has several of its characteristics that make it more or less specific and recognizable. However, the reliability of these characteristics is usually low when viewed separately. Reliability increases proportionally to the number of analyzed characteristics and their interrelationships are integral parts of a comprehensive clinical picture.
Attentive clinical examination of the oral cavity majority can find the cause of dental pain such as dental caries, dental trauma, fractures of the crown or root, old and / or inadequate fillings, denuded dentin and others. For odontogenic pain characteristic that is often during the test can be deliberately provoke the painful stimulus, for example, by directing a jet of cold air or water to the suspected tooth. Given the fact that the cause of dental pain single tooth, the pain is unilateral, or engages himself one side of the jaw and often it is possible to accurately localize though not necessarily always. Suspicious tooth may be sensitive to changes in temperature and pressure (bite or percussion). The tooth pain relief can be achieved by using a local anesthetic. One of the characteristics of dental pain and its limited duration (days or weeks). Sue Does the patient on chronic pain that lasts for weeks and / or months, and it is unchanged character, we must examine the possibility that the pain neodontogenog origin.
In order to properly dentist diagnosed dental pain, must first take dental history which should include patient subjective description of the pain. The patient should be given information about the characteristics of pain (dull, sharp, drumming, shooting, stabbing, throbbing), its duration, frequency of occurrence, the method of generation and the like. The data from the medical history should be complemented by a clinical examination of the oral cavity, inspection, palpation, percussion, heat test, test the vitality of dental pulp, and X-rays suspicious teeth or parts of teeth.
What can mimic odontogenic pain?
Although odontogenic pain has some of his more or less specific features, it is not always possible to say with certainty that the individual teeth cause pain in the face and lips cavity. Orofacial pain can have many of his nonodontogenic causes about which particular care should be taken when setting up a differential diagnosis. Neodontogena pain may have musculoskeletal, neuropathic, neurovascular, inflammatory, systemic and psychogenic background. Thus a wide range of possible causes of pain in the face and mouth the dentist can be a diagnostic challenge, but by taking a thorough dental history, clinical examination and application of appropriate tests most causes of dental pain can be properly identified.
What is dentin pain?
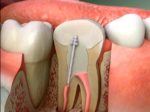
According to Bender pain of odontogenic origin implies dentin and pulp pain. Dentin and pulp pain occur as a result of stimulation of two different nerve fibers at different places in the pulp (the soft gum tissue surrounded by dentin and placed in the pulp chamber inside the tooth). Terminations brzoprovodnih A-delta fibers are mostly located on the border of the pulp and dentin, which means on the periphery of the pulp. These endings penetrate the dentinal tubules in depth from 150 to 200 microns. Nearly all of the A-delta fibers are located in the crown area of the pulp, and are arranged densely in the area of the pulpal horns. On the other hand, sporoprovodna C-fibers are located in the deeper layers of pulp and permeate zone rich cells. Stimulus A-delta fibers causes a sharp, swift and stabbing pain (pain dentin), while C-fiber stimulation causes a dull, diffuse pain (pain pulp).
The cause of dental pain are changes in the dentin (the hard tooth tissue located under the enamel in the tooth crown or below the dental cement in the root canal). Do hypersensitivity is due to exposure and opening the dentinal tubules (tube), which conductor (conductor) pain, and become susceptible to external factors.
To Exposure of the dentine tubules external factors may occur due to wear of hard dental tissue, but also iatrogenic: unprofessional dental work, inadequate therapeutic preparation, unsuitable application materials for filling teeth and so on. Spending hard dental tissue (abrasion, attrition, erosion) regardless of the cause can lead to exposure of dentinal tubules external influences, resulting in hypersensitivity dentin and painful sensations which can sometimes be so severe that the patient requires that his tooth pulled out. As this is a healthy or too sensitive teeth, the patient then we must explain what it is, answer it by tooth extraction and reduce his sensitivity to painful stimuli and thus save the tooth.
The pulp pain
Pulp pain or pulpalgija is pain that occurs stimulus tooth pulp. Each local inflammation within the pulp chamber causes pain which can manifest itself in different ways. According to Melissa and associates characteristics of pulp pain are:
- pain is oscillating character as time increases or weak
- local provocation (heat, cold, pressure) increase the pain
- clinically and radiologically is possible to find the causes of pain (caries, fracture, etc.).
- Endodontic treatment pain is removed by
- local anesthesia eliminates pain.
pulp pain can manifest as: return (reversible) pulpitis, irreversible (irreversible) pulpitis, acute apical periodontitis and acute apical abscess.
Return (reversible) pulpitis is defined as inflammation of the pulp of lower intensity. Mild and short-irritating stimuli such as initial caries lesions, cervical erosion, occlusal attrition, enamel fractures and numerous dental procedures (eg, curettage periodontal) lead to exposure of dentinal tubules, which can cause reversible pulpitis. Reversible pulpitis usually asymptomatic. But if there are symptoms, then have a specific form of appearance. Stimuli such as hot or cold liquid or air cause a sharp but transient pain. By removing these stimuli, which usually do not cause unpleasant sensations, pain immediately disappears. Heat and cold cause different pain responses in healthy pulp. When the heat source is placed on the tooth, there is a delayed initial response, and the intensity of the pain increases proportionately to the increase of temperature.
On the other hand, the pain caused by cold stimulation occurs now, except that it is decreased as to whether the cold stimulus savings. Based on these observations it can be concluded that the response and the healthy and the sick pulp depends on changes in intrapulpnom pressure.
I irreversible (irreversible) pulpitis is usually asymptomatic or a patient appear only mild symptoms. On the other hand, some patients irreversible pulpitis may be associated with temporary or permanent episodes of spontaneous pain (not caused by external stimuli). The pain of irreversible pulpitis can vary from sharp to dull, may be localized or diffuse and this can take several minutes or several hours. Localization pulp pain is much more difficult than determining the place of pain periradicular origin and all it difficult to localize as intense. The application of external stimuli such as heat or cold can cause prolonged pain. In the presence of extreme pain, the pulp response differs depending on whether it is healthy or inflamed. Eg., By applying heat to the tooth with irreversible pulpitis leads to instantaneous painful stimulus, while the application of cold can cause prolonged pain. Sometimes, the application of cold in patients with painful irreversible pulpitis causes vasoconstriction and decrease the pulp pressure, which reduces pain. In odontogenic reflected pain, pain that comes from teeth can be reflected on the other orofacial structures and conceal the real cause of pain. It is not often that the pain caused by pathological changes in the pulp of one side of the jaw moves to the opposite page faces. Odontogena reflected the pain often associated with irreversible pulpitis. The most frequently manifests itself in the back parts of the upper or lower jaw.
Acute apical periodontitis resulting expansion of pulp inflammation in periradicular area. Irritating factors are mediators of inflammation from irreversibly inflamed pulp, bacterial toxins from necrotic pulp, chemicals (washing solution and disinfecting root canal), excessive fill, excessive instrumentation and overcharging root canal. Symptoms of acute apical periodontitis vary from medium to express spontaneous pain, to pain when chewing and occlusal contacts. If acute apical periodontitis result of inflammation of the pulp, possible sensitivity to hot and cold and sensitivity to electrical stimuli. On the other hand, if the acute apical periodontitis result of necrosis of the pulp, the tooth will not show signs of vitality. Pressing teeth and percussion can cause pain. Radiographic can be observed thickening of the periodontal ligament, but he can often stay and a full-size and fully intact. Histologically, in the apex of the tooth see localized accumulation of polymorphonuclear leukocytes and macrophages. Sometimes it is possible to spot and less area liquefaction necrosis (abscess). Although bone resorption and roots can be histological, radiological usually not visible. Treatment consists of removing irritating factors that led to the onset of acute apical periodontitis.
Occasionally (asymptomatic) apical periodontitis occurs when dental pulp begins to gradually die out without causing symptoms and slowly release harmful inflammatory agents low pathogenicity or low concentrations. Occasionally (asymptomatic) apical periodontitis is very often the result of a failed endodontic treatment that remains concealed until symptoms appear. Any chronic back easily exceed the acute stage when infection occurs with existing new, when reduced immunity, or when to increase the virulence of microorganisms. This type of apical periodontitis is associated with resorption radiological periradicular alveolar bone. Patients usually do not complain of painful stimuli, and to test the vitality react badly because they do not cause painful sensations. Eventually, if there is a perforation of the alveolar bone, palpation of the perforation can cause discomfort and bad pain.
Acute (symptomatic) apical abscess may be localized or diffuse liquefaction lesion that destroys periradicular tissue and can be a strong inflammatory response to microbial or nemikrobne irritants arising from necrotic pulp. Depending on the severity of the reaction, patients with acute apical abscess usually feel moderate to severe pain and have swelling. Sometimes it can show and systemic manifestations of infectious processes such as fever, weakness or leukocytosis. How to acute apical abscess comes only if the necrotic pulp, tooth shows no effect on the thermal and electrical stimuli. But these teeth are often sensitive to percussion and palpation. Depending on the degree of destruction of periradicular tissue, radiographic findings vary from expansion of periodontal crack (rarely) to the clearly expressed resorptive lesions (often).
What is the treatment odontogenic pain?
The treatment methods of dental pain depends on its cause. If the cause of dental caries, the treatment is restorative, which includes cleaning of dental caries, dental pulp protection and restoration. In dental trauma as the cause of dental pain, disposed of traumatic tooth, but depending on the trauma can range from putting bandages dentin and pulp protection to endodontic procedure and immobilization of teeth. Dentin hypersensitivity tooth pain and heal the closure of dentinal tubules, preventing transmission of external stimuli to the pulp. More recent attempts to reduce dentine hypersensitivity are going in the direction of remineralization and occluding the open dentinal tubules. For this purpose apply to preparations based on calcium-sodium fosfosilikata who have the ability to quick release of calcium, phosphate, sodium and silicate and formation of a new layer on the surface of the dentin, which closes open dentinal tubules. Pulp pain, depending on the state of pulp, may require only pulp capping (directly or indirectly) the appropriate preparations, but also completely endodontic dental treatment, including treatment, disinfection and root canal filling. Sometimes endodontic treatment must be combined with endodontic-surgical procedures.
Depending on the cause of dental pain and medical condition of the patient, the dentist may recommend taking analgesics, antipyretics and antibiotics.
How to prevent dental pain?
Avoiding the causes of dental pain is the most effective way of preventing her. This primarily refers to dental caries as the most common reason for the appearance of dental pain. With regular and proper oral care and teeth, adequate nutrition and control visits to the dentist can significantly reduce the incidence of dental caries, and thus the need for endodontic treatment. By avoiding the consumption of drinks that have erosive effects (carbonated and / or highly acidic drinks) reduces the risk of dental erosion, which is one of the most common causes of dentin hypersensitivity. The application sports mouthguard, teeth are protected from trauma and injury, thus preventing and dentin and pulp pain.
Conclusion
Odontogenic pain is one of the most common types of pain in the orofacial area, and its most common cause of dental caries. Odontogena pain can sometimes be recognized as neodontogena pain and vice versa. Preventive dental oral hygiene measures are usually preventable causes of dental pain.