AIDS or Acquired Immunodeficiency Syndrome is a disease that affects the immune system. This is a contagious and still incurable viral disease for which a vaccine has not yet been found. AIDS is caused by the virus of human immunodeficiency (HIV-1, HIV-2) which is a species of retrovirus. HIV-1 is most commonly found in patients in Europe, the US and Central Africa, while HIV-2 occurs in patients in West Africa.
 The virus attacks the immune system and the central nervous system. Within the immune system T4-lymphocytes are affected with virus. These cells play an important role in the functioning of the immune system. After infection with HIV, T4 cells lose their function in the immune defense of the organism, and soon after the multiplication of the virus are killed, thus their number in the body significantly decreases.
The virus attacks the immune system and the central nervous system. Within the immune system T4-lymphocytes are affected with virus. These cells play an important role in the functioning of the immune system. After infection with HIV, T4 cells lose their function in the immune defense of the organism, and soon after the multiplication of the virus are killed, thus their number in the body significantly decreases.
Within the HIV infection three phases can be distinguished: early acute phase, secondary chronic phase and final phase or a crisis.
The early acute phase is the response of the infected organism to infection by HIV, and it is characterized by replication of the virus in the organism and antiviral immune response. In the secondary chronic phase the virus begins to destroy cells of the immune system. This phase can last for months, even years, depending on the speed of propagation of the virus and effective response of the immune system of the organism. Sick individuals either do not have any symptoms or these symptoms are very non-specific, such as increased size of lymph nodes throughout the body. When the increase of the lymph nodes becomes extreme and followed by general symptoms such as an increased body temperature, rash, weight loss and fatigue, it means that there has been a failure of the immune system and the final phase of illness or crisis is beginning. As it’s predecessors are considered cervical lymphadenopathy, oropharyngeal candidiasis and hairy leukoplakia. During the crisis the immune system completely breaks down, opportunistic infections (such as Pneumocystis carinii pneumonia, Mycobacterium infections) and secondary malignant tumors appear (such as Kaposi’s sarcoma). In this third faze clinically clear signs of damage to the nervous system are also present.
HIV is a disease that occurs worldwide and it is estimated that there are more than 35 million people infected with HIV!
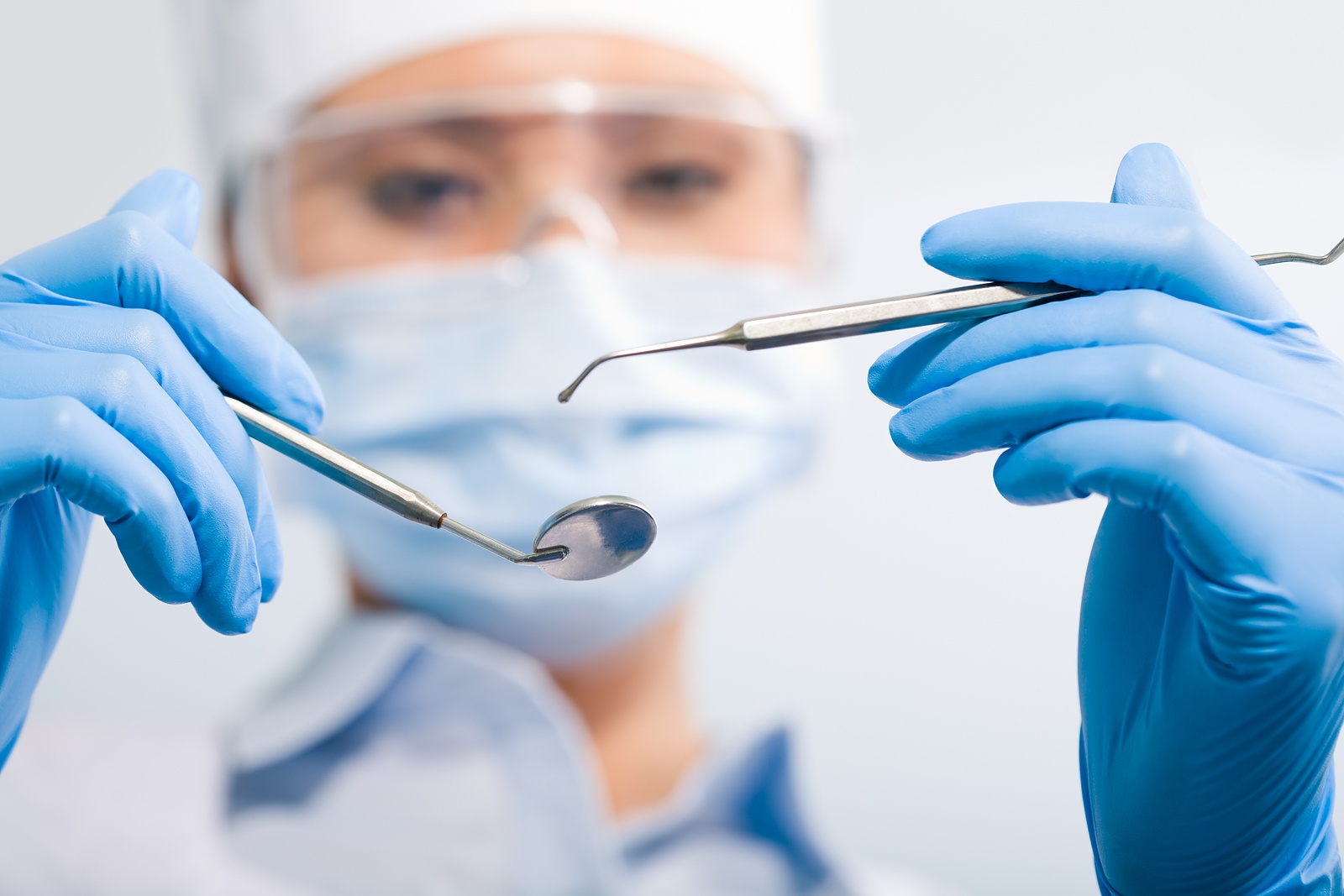
 The diagnosis is made based on the results of laboratory tests (ELISA, Western blot, PCR, RIPA, etc.) which detect the virus and determine the number of T4-lymphocytes in the blood, the presence of opportunistic infections and malignancies that occur during the disease. The presence of HIV antibodies in the organism is considered to be a sign of infection, but their absence does not necessarily mean that the person is not infected with HIV because there may be a relatively long latency period (the period between infection with a virus and the onset of symptoms). It is believed that in Europe 30 percent of all people infected with HIV are not aware that they are seropositive (have a positive result in a test of blood serum for the presence of HIV virus). Because the disease can remain latent for a long time, it is important to recognize other symptoms and signs that may be associated with HIV infection. Some of these signs can manifest in the oral cavity, therefore the role of the dentist in the early detection of HIV disease is extremely important.
The diagnosis is made based on the results of laboratory tests (ELISA, Western blot, PCR, RIPA, etc.) which detect the virus and determine the number of T4-lymphocytes in the blood, the presence of opportunistic infections and malignancies that occur during the disease. The presence of HIV antibodies in the organism is considered to be a sign of infection, but their absence does not necessarily mean that the person is not infected with HIV because there may be a relatively long latency period (the period between infection with a virus and the onset of symptoms). It is believed that in Europe 30 percent of all people infected with HIV are not aware that they are seropositive (have a positive result in a test of blood serum for the presence of HIV virus). Because the disease can remain latent for a long time, it is important to recognize other symptoms and signs that may be associated with HIV infection. Some of these signs can manifest in the oral cavity, therefore the role of the dentist in the early detection of HIV disease is extremely important.
HIV virus is transmitted by blood and body fluids (semen, vaginal, saliva) from the infected person to healthy people!
HIV virus can be transmitted during high-risk homosexual, bisexual and heterosexual contact when person has a large number of sexual partners or sexual relations with strangers, during sexual contact with permanent HIV-positive partner, with intravenous injections of drugs by sharing infected needles and with blood transfusion by receiving infected blood. Also, a child can get HIV virus from infected mother through the placenta or breastfeeding. People with hemophilia can also get infected with the HIV virus. Although less common due to the protective effects of saliva, the HIV virus can also be transmitted by oral-genital sexual contact. But if there is an oral lesion already present in the mouth, then transmission of the virus can be accelerated.
 To prevent AIDS disease many centers for anonymous and free HIV counseling and testing operate worldwide. Unfortunately, scientists have not yet discovered neither a vaccine that would prevent nor drugs that could cure this disease. However, early detection of the disease and the application of certain drugs (antivirals) can slow down the progression of the disease. During the administration of drugs for the treatment of primary disease, patient should always take into account their possible side effects that may occur in the oral cavity. Some of them may affect the secretion of saliva and cause dry mouth (Xerostomia), which can be disastrous for normal physiological cleaning and rinsing of the mouth with saliva and highly favors the development of dental caries, tartar buildups and periodontal diseases.
To prevent AIDS disease many centers for anonymous and free HIV counseling and testing operate worldwide. Unfortunately, scientists have not yet discovered neither a vaccine that would prevent nor drugs that could cure this disease. However, early detection of the disease and the application of certain drugs (antivirals) can slow down the progression of the disease. During the administration of drugs for the treatment of primary disease, patient should always take into account their possible side effects that may occur in the oral cavity. Some of them may affect the secretion of saliva and cause dry mouth (Xerostomia), which can be disastrous for normal physiological cleaning and rinsing of the mouth with saliva and highly favors the development of dental caries, tartar buildups and periodontal diseases.
Oral manifestations of HIV infection
Due to the weakening of the immune system of the entire organism, in the oral cavity HIV infection can manifest with fungal, bacterial and viral infections, malignant neoplasms, non-specific changes (such as aphthous ulcerations) and neurological disorders (such as nerve paresis and neuralgia).
The role of the dentist is especially important in the early detection of signs of HIV infection because it is considered that, in more than 90% of AIDS patients, at least one oral symptom of this disease can be found in the mouth.
Among the fungal infections there are oral and esophageal candidiasis that can occur in various forms. The most common is pseudomembranous candidiasis, which mostly affects the lining of the cheeks, dorsum of tongue and palate. This fungal infection can spread from the mouth to the mucosa of the respiratory and digestive systems and on the facial skin around the mouth. In addition to oral candidiasis, other fungal infections may occur such as histoplasmosis and aspergillosis.
Inflammation of the gums (gingivitis) and periodontal tissue (periodontitis) are the most common types of bacterial infections that can occur as a result of infection with HIV. The decline of immune capacity of the body can also lead to the activation of periapical lesions around the apex of a tooth root. Extra pulmonary or disseminated tuberculosis (tuberculosis infection which is not located in lungs) can also occur in the oral cavity and arouse the suspicion of HIV infection.
The most common types of viral infections that appear in HIV infected patients are infections with herpes simplex virus, varicella zoster virus, cytomegalovirus, Epstein-Barr virus, papilloma virus and poxvirus. Herpes simplex virus infection can manifest as primary herpetic gingivostomatitis or recurrent herpes labialis (oral herpes). In case of infection with cytomegalovirus ulcerations of the mucous membranes of the mouth and inflammation of the salivary glands (sialadenitis) may occur. Ulcerations of the oral mucosa can also appear in infection with Epstein-Barr virus, which may be accompanied by the appearance of petechiae and hairy leukoplakia. HIV induced papilloma virus infections in the oral cavity may manifest as oral condyloma, leukoplakia or epithelial hyperplasia.
In the group of malignant neoplasms whose occurrence is associated with HIV infection most common are Kaposi’s sarcoma, non-Hodgkin’s lymphoma (Burkitt’s lymphoma) and squamous cell carcinoma. Kaposi’s sarcoma is a malignant, slow-growing malignant growth in the oral cavity which is usually located on the palate and may be purple, blue, red or brown. This tumor usually does not have tendency to metastasize and it is considered that it does not cause death. Non-Hodgkin’s lymphoma occurs in young adults, especially those infected with Epstein-Barr virus. The tumor lesions can be found in the salivary glands and jaws. Squamous cell carcinoma (carcinoma planocellulare) is the most common of all cancers of the oral cavity. It occurs as a painless ulceration, fissure or white keratosis on the tongue, lower lip, the bottom of the mouth, face or on the palatine tonsils.
One product that can help with removing tonsil stones is a Waterpik water flosser.
 Dental care of people with HIV
Dental care of people with HIV
Treatment of pathological changes that manifest in the oral cavity and are associated with HIV infection is carried out according to their causes and symptoms. With this approach it is possible to reduce pain, have tooth pain relief, restore disrupted function of the oral cavity and prevent new infections and the emergence of other oral complications. Good oral health positively affects the quality of life of patients affected with HIV.
Since AIDS is a contagious disease which has no cure, and it can be further transferred by implementation of dental care, the infected patient is required to meet the dentist with the fact that he is infected with HIV and the current situation of his disease. This may need to be supported by the latest laboratory findings. All information about health condition that a patient entrusted to the dentist are considered as professional secrecy. The dentist should provide to patients with AIDS the best possible dental care, but also is obligated to protect other patients, members of the dental team and himself from possible infection!
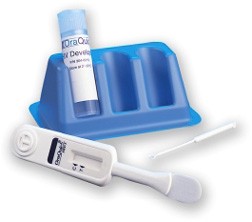 As dentists and dental hygienists belong to the group of high risk professions for HIV infection, the developed countries of Europe and the United States are increasingly introducing in dental practice so-called rapid tests for the detection of HIV infection that provide results within twenty minutes. The tests are based on ELISA technology and can detect antibodies to HIV-1 and HIV-2 viruses in the gingival fluid and blood. Sensitivity of the test is between 98 and 100 percent. It is important that each dental patient is treated as potentially infected person, which means that during the work with each patient suitable protective measures and corresponding measures of sterilization and disinfection must be applied.
As dentists and dental hygienists belong to the group of high risk professions for HIV infection, the developed countries of Europe and the United States are increasingly introducing in dental practice so-called rapid tests for the detection of HIV infection that provide results within twenty minutes. The tests are based on ELISA technology and can detect antibodies to HIV-1 and HIV-2 viruses in the gingival fluid and blood. Sensitivity of the test is between 98 and 100 percent. It is important that each dental patient is treated as potentially infected person, which means that during the work with each patient suitable protective measures and corresponding measures of sterilization and disinfection must be applied.
However, patients with incurable diseases such as AIDS are still socially unacceptable. Since it is very difficult to find a dentist who is willing to treat such a person, these patients sadly keep quiet about details of their illness. Although such an approach is understandable, it is considered socially irresponsible behavior because of the possibility of spreading the infection. Dentists are required to treat all patients, but with different justifications that can be relatively easy to avoid. On the other hand, due to this approach, some of infected patients avoid dental visits which worsens their oral health. It is estimated that about one-third of people with AIDS has serious dental problems that have been caused by the weakening of their immune system. Untreated oral lesions can cause problems with eating and chewing, which leads to weight loss and malnutrition. Therefore, inadequate dental care and neglect of oral health can badly affect the development of the disease and threaten the life of a patient. In an attempt to solve this problem, the American Dental Association (ADA) in 2004 introduced dental case manager that connects individual patient with an incurable infectious diseases with a dentist who is willing to provide appropriate dental care.
In achieving and preserving good oral health of people affected by AIDS, an extremely important role has the dentist’s knowledge about the disease. This emphasizes the importance of knowledge and education of patients and dental staff about AIDS.
 Affected persons should be educated about the disease manifestations in the oral cavity, their treatment and the appropriate ways of maintaining oral hygiene. Such a preventive approach not only improves the quality of life of patients and indirectly their family, but it is possible to save up some money for the health system as well. On the other hand, dentists, dental team members and dental students should learn how to deal with patients suffering from AIDS, how to provide them the best possible dental care and do not endanger neither their health nor the health of other patients. With modern medical or dental training, appropriate psychological approach and appropriate social sensitivity, it is possible to reduce the stigmatization of affected individuals in society and provide them a sense of equality and acceptance.
Affected persons should be educated about the disease manifestations in the oral cavity, their treatment and the appropriate ways of maintaining oral hygiene. Such a preventive approach not only improves the quality of life of patients and indirectly their family, but it is possible to save up some money for the health system as well. On the other hand, dentists, dental team members and dental students should learn how to deal with patients suffering from AIDS, how to provide them the best possible dental care and do not endanger neither their health nor the health of other patients. With modern medical or dental training, appropriate psychological approach and appropriate social sensitivity, it is possible to reduce the stigmatization of affected individuals in society and provide them a sense of equality and acceptance.
Conclusion
AIDS is contagious and still incurable disease whose signs can be noticed in the oral cavity. Because of the direct contact with the patient’s blood and saliva, dentists and dental hygienists belong to the high risk group for HIV infection since they can be infected with HIV during dental treatment. Although patients are required to meet the dentist with their state of health in order to prevent the spread of infection during the implementation of dental procedures, they sometimes fail to do so. Therefore, every dental patient should be considered as potentially contaminated. Preventing the spread of HIV infection is based on avoiding risky sexual relationships, personally and socially responsible behavior and education about the disease.